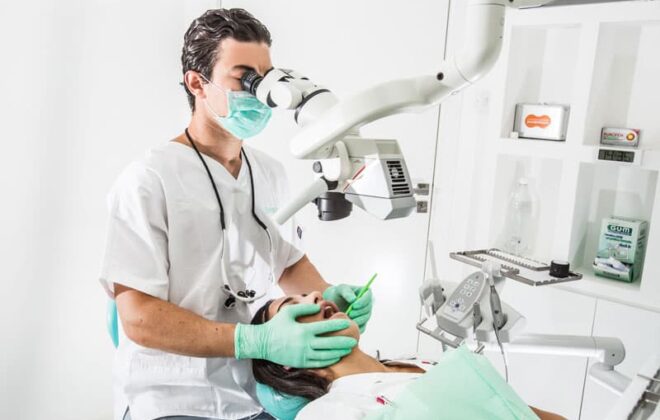
5 Most Common Procedures an Endodontist Works On
Some patients often ask what the difference is between an endodontist and a dentist. Essentially, an endodontist is a specialized dentist who has finished an extra two or more years of education beyond dental school. Through this additional training, the endodontist has gained in-depth knowledge in several specialties, including root canals (among other procedures). This is why some people refer to endodontists as “root canal dentists.” But that’s just part of the story. Read on to learn more about the cases and procedures for which your dentist may refer you to an endodontist.
It’s a Collaboration Between Dental Specialists
When you get sick, you go to your family doctor, typically a general practitioner. When she or he narrows down what the issue is, a course of treatment can be prescribed.
There are times, however, when a specialist is called for. If your family doctor determines (or suspects) that your symptoms are related to your central nervous system, for example, you’ll likely be referred to a specialist called a neurologist, who focuses on treating disorders of the nervous system.
Similarly, your dentist is the first person you turn to when you are experiencing any type of dental issue. In the vast majority of cases, your family dentist will diagnose the problem and provide treatment at his or her dental clinic.
There are occasions, though, when a dental patient will require additional expertise by a different dental specialist. One such specialist is an endodontist, and your dentist may refer you to one for certain procedures, including the following. (Be aware, though, that your dentist may have the background to handle these procedures in her or his office as well.)
Root Canal
A root canal is needed when pulp tissue deep inside a tooth becomes infected or inflamed, resulting in symptoms of (sometimes significant) pain. The affected tissue is made up of connective tissues, blood vessels, and nerves; an infection in this area needs to be treated before it grows into an even bigger problem.
Root canal therapy is done to save your natural tooth and avoid bridges or implants, as well as relieve the symptoms of pain that are present. Even though it takes specialized training for a dentist to be able to perform a root canal, this procedure is very common, with over 14 million successfully completed each year. As with a filling, an anesthetic is administered for the purposes of numbing the area. The infected pulp tissue is removed, and then the canals are thoroughly cleaned and disinfected. The root canals are then filled with an inert, biocompatible substance. At the end of the procedure, the tooth is sealed off to prevent future infections.
In many cases, a dental crown is fitted over the affected tooth to further protect it. The crown goes over the surface of your tooth, like a cap; you still have your original, natural tooth in place, but with the infection removed and the structure reinforced!
Additional Root-Level Infections
In the majority of cases, a root canal is successful and no further treatment is required. In some cases, though, the pain may return, and a new infection may develop, perhaps in small branches of the root canals. In these instances, additional treatments may be needed by an endodontist to eliminate the infection and relieve pain related to this new flare-up. Each patient is treated on a case-by-case basis; your dentist and your endodontist (who may well be the same person!) will carefully go over options with you should pain return at some point after your root canal procedure.
Endodontic Surgery
An apicoectomy is a form of surgery that an endodontist may turn to when the infection is deep in the bone. Instead of reaching it through the tooth itself, the infection is accessed and removed through the gum tissues. A surgical incision is made to reach the infection or abscess found at the tip of the tooth’s root; the infected tissue is removed, and a filling material is placed at the tip to prevent the region from being reinfected.
Tooth Fractures
Some fractures are small and located only on the surface, and these usually can be remedied via a filling or bonding. There are cases, however, when the crack is bigger and deeper, causing a significant level of pain and creating problems when chewing. The resulting pressure and temperature sensitivities can become too much to handle.
In a cracked tooth, the soft tissues inside can become irritated; with the nerves in this region agitated, the pain can escalate. An endodontist can treat a cracked tooth to relieve pain symptoms. From a split tooth to a vertical root fracture, and any other type of crack, an endodontist will take measures to repair the damage and relieve the pain.
Procedures That Address Injuries
In a traumatic injury, a tooth may become dislodged. It may be pushed out, in, or out of place in some way, affecting not only the tooth but the region around it, too. In these cases, an endodontist can be of tremendous service.
Depending on the situation, treatment may involve replacing and restoring a loose tooth, treating any other damage the mouth has experienced, and possibly doing a root canal. If you are involved in an injury or accident that has affected your teeth in any way, seek help from a dentist immediately. Emergency dental care is available for these instances, and seeing a dentist right away (rather than waiting) can make all the difference between saving or losing the tooth.
Article originally appeared at: https://www.merrittmilldental.com/
Author: Merritt Mill Dental Associates