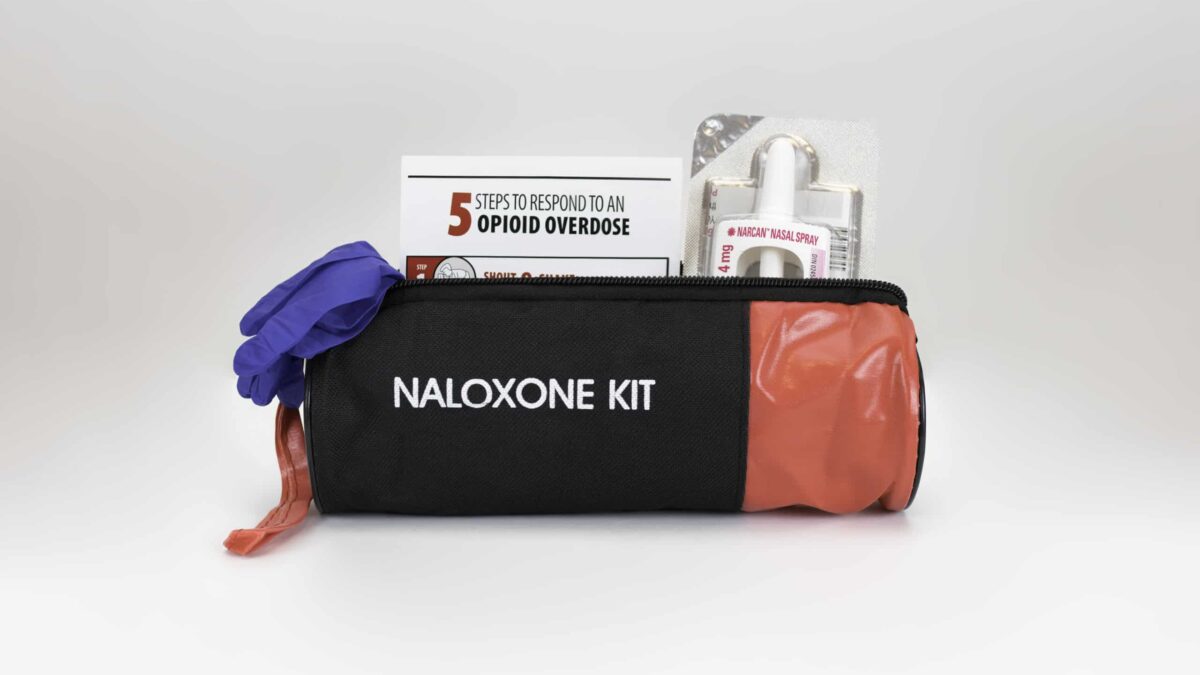
Naloxone – The Eighth Drug in the Dental Emergency Kit?
The COVID-19 pandemic may have been grabbing the headlines in recent months, but there is another epidemic that has not gone away: The Opioid Crisis. And though we may not be reading about it in the news, we are still seeing a significant number of overdose deaths associated with opioids, both licit and illicit.
As oral healthcare professionals, one of the challenges for dentists is understanding how they can be part of the solution.
In a recent article published in General Dentistry (May-June 2020), Dr. Mark Donaldson, Senior Executive Director at Vizient, speaks about the opioid antagonist Naloxone; and explains why dentists should consider including it in the Dental Emergency Kit.
Naloxone has been around since 1961 when Jack Fishman, a chemist working for a small private lab in New York City, was looking for a medication to combat the side effects of narcotics, specifically constipation. Fishman subsequently stumbled upon Naloxone, a powerful medication used to block the effects of opioids that has gone on to save thousands of lives.
In 1983, Naloxone was added to the WHO list of essential medications, and has since become a household name, carried by medical emergency teams all over the world. And although originally developed as an injectable drug, in recent times, pharmaceutical companies have developed intra-nasal sprays and auto-injector formulations that are accessible without prescription in Canada.
But why should a dentist include Naloxone in their Dental Emergency Kit?
Dr. Donaldson considers a scenario where a patient requires sedation and then loses consciousness: “If the reversal agent for the sedative does not work, not only are you calling 911 but you probably want to give that patient Naloxone because more than likely they have taken some kind of narcotic to calm their nerves and didn’t tell the dentist. And the combination of the narcotic and the sedative has caused an unintended overdose. Since our patients don’t always tell us the truth, it makes great sense for dental offices to consider the addition of Naloxone to their kit.”
“Since our patients don’t always tell us the truth, it makes great sense for dental offices to consider the addition of Naloxone to their kit.”
In the United States, regulations are changing. The Washington State Board of Dentistry guidelines now dictate that a dentist who is prescribing opioids for post-operative pain must consider either co-prescribing Naloxone, or at least direct the patient to discuss with their pharmacist whether they need access to Naloxone.
“It wouldn’t surprise me if Dental Colleges in Canada start to look at the changing regulations in the US and consider the same opportunity,” says Dr. Donaldson. “This creates an additional hurdle for dentists in prescribing opioids and I think that is a good thing. At the end of the day our goal is appropriate prescribing. To keep the patient safe and create a conduit for them to have access to a reversal agent if required.”
Author:
Chiraz Guessaier, CDA Oasis Manager
Article originally appeared at: http://oasisdiscussions.ca/2020/06/02/naloxone-the-eighth-drug-in-the-dental-emergency-kit/