Research Finds Minimal COVID-19 Risk at Dentist
As dentists reopened in late spring, very few got Covid-19, survey finds
Early on in the pandemic, it was widely believed that dentists would be at high risk of contracting Covid-19.
Rates of Covid-19 among dentists were low in the late spring, as dental practices reopened and patients returned, a report published Thursday from the American Dental Association suggests.
Researchers conducted a nationwide survey June 8 with responses from more than 2,000 dentists from across the country. Just 0.9 percent, they found, had either confirmed or probable cases of Covid-19.
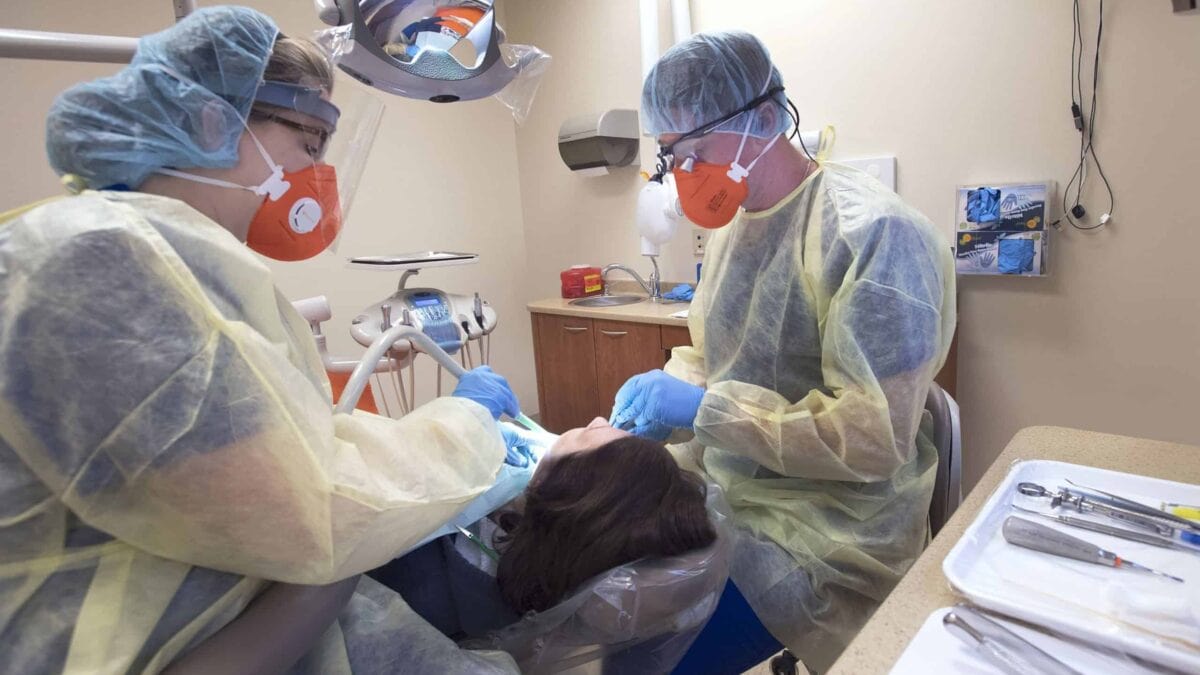
Early on in the pandemic, it was widely believed that dentists would be at high risk of contracting Covid-19, as their work puts them in very close contact with patients, and many of their procedures, which involve water and air spray, could generate virus-laden aerosol particles.
The survey also found that virtually all of the dentists — 99.7 percent — were using what was referred to as “enhanced infection control procedures.” These included screening protocols for patients and disinfection practices.
However, while nearly all dentists reported some use of personal protective equipment, only 73 percent of dentists reported wearing PPE in accordance with national guidance from the Centers for Disease Control and Prevention. This required the use of a surgical mask, a gown, gloves and eye protection during procedures not expected to produce aerosols and use of an N95 respirator for aerosol-generating procedures.
Cameron Estrich, a health data analyst at the ADA and lead author of the study, said that she was surprised by two things in her research: the low rate of infection, and the extremely high adoption of infection control measures.
“Pretty much all of the dentists that we surveyed had really stepped up their infection control and prevention procedures,” she said. “They had shut down their practices for a few months to get these all in place.”
“It looks at a time when the pandemic was at its height and the experiences in the dental practices were probably more or less limited in terms of how much aerosols that we’re generating,” Roykh, who was not involved with the ADA report, said.
In New York, for example, dentists were not allowed to fully reopen until May 31, just over a week before the survey was sent out.
Roykh said while these findings are preliminary, they mirror what she has seen in her dental practice.
“Our experience with this specific pandemic shows that when we are compliant with good PPE measures, and health and safety controls are in place, that we are generally able to keep our workforce safe,” she said.
Renee Anthony, a professor of occupational and environmental health at the University of Iowa, said that she is looking for data on infection rates of patients who have visited dental offices.
“While dentists are able to protect themselves during and between patient treatment, the patients must receive treatment without wearing a face covering,” Anthony, who was also not involved with the report, said.
Anthony said the big question that remains is whether or not these measures taken will prohibit the spread of the virus between patients who are visiting at different times. (The ADA study found that, for the cases among dentists for which they were able to do contact tracing, the dentists were infected not at work but in the community.)
“A critical unanswered question is whether the infection control practices explored in this paper are sufficient to reduce the patient-patient transmission if this virus, on smaller respirable particles, remains in the treatment rooms between exams/procedures,” she said.
Author: Akshay Syal
Article originally appeared at: http://nbcnews.com